The First Time I....Walked in Over Two Years
 |
| March 29, 2011Standing for the first time with the help of Jim, my PT |
I fell in Dec. 2008 and could neither stand nor walk afterward. MRIs, X-rays, Doppler imaging, and nerve conduction studies, all showed nothing that would mean I couldn't walk. That led doctors to make the only reasonable conclusion, it was thought to be a soft tissue injury. As such, it may or may not heal and if it did, might be slow healing.
I spent months at Grand Strand Regional Medical Center with other problems, chronic infections of varying natures, and was pretty much unable to move on my own. I think part of my lack of movement was the fact that I was off of ALL of my RA medications because of the infections I kept getting. They'd get rid of one infection only to have a different crop up. Another affect of being off of my medications was that just being touched caused me immense pain. Thankfully, I do not remember much of that time.
I remember parts of that time. One time I remember is being told that I'd likely never walk again. Another was that I'd likely not live outside of a hospital or nursing home. One doctor even went so far as to very rudely state that I was "nothing but a terminal patient." Needless to say, that doctor was never allowed back into my room. The hospital PT gave me a bit different of a prognosis. His assessment was that it would take 2-3 years of daily, intensive physical therapy to stand let alone walk, IF it were possible.
On Nov. 22, 2009 I was transferred to Conway Manor nursing home. In the first few days I was there, the head of PT came to do an evaluation but we never started PT. At the time, I was too ill to care. The first week there I had such a horrible problem with nausea, vomiting and not having an appetite. I know part of it was a bit of depression and worry over the move. That was to be expected. I moved from the known to the unknown, not knowing anyone there made it hard to be comfortable. I had gotten to know the hospital staff and felt comfortable with them. I knew how each person worked and what to expect. So not knowing. especially being pretty much 100% dependent on people, was hard. It also did not help that because she did not know my reaction to milk, a nurse mixed my crushed medications in with some milk and put it in my stomach tube. That was not a good thing. I couldn't tell her to stop because literally the moment the milk hit my stomach, it came up. It's hard to talk while throwing up. It also came back out the tube which means I think I got her twice.
At my first care plan review, I finally questioned why PT had never been started. Of course that needed looked into. I was later told that I said I did NOT want PT. I do not ever recall saying I didn't want PT. If someone came in during the days I was sick, I wouldn't have said I didn't want it, I'd have said I was sick and didn't think I could do it while sick, but I'd not have refused it completely. So I started PT. I'd not had any exercise in at least two years because before getting sick I wasn't doing all that well and had been pretty sedentary since I'd had a high level of disease activity. My first day in PT, I was put in a group of residents who were doing various chair exercises. No one cautioned me to hold back and not try to keep up with the others in the group and I was not at 100% yet in thinking from the months I was out of it, so I didn't really stop to think how I'd be affected by doing 30-40 repetitions of 6-8 exercises. I kept up with the others, I was kinda proud of that. That bit of pride only lasted until a little while later. I paid for that bit of pride in that I ended up in bed for approximately 3 weeks, barely able to move on my own. I was miserable.
I asked about restorative therapy. They did things with residents who didn't quite need a therapist's help but still needed assistance. For some residents, in order to get better at walking, they needed someone to walk with them and hold onto a gait belt the person wore to keep them safe. For some who were bed-bound, restorative kept their arms and legs exercised by doing gentle stretching and range of motion (ROM) exercises. That was exactly what I needed until I was a bit stronger and able to be more active. I was supposed to get restorative therapy five days a week. But it was written down wrong in the orders and only written for three days, but knowing I'd asked for five, the restorative therapy staff tried to be there all five days. The only issue was on days they pulled restorative to the floor to work as a CNA. They were trained as CNAs and so when an area was short a CNA, they had restorative to be able to help. It's not the fault of the staff member doing my restorative exercises but in the approximately 6 mo. they worked with me, the only changes made were to add to the number of repetitions I did, once we got me to the point I was able to do all of the exercises we discussed in the beginning. No one ever re-evaluated me to see if we needed to add anything else. During the times restorative worked on the floor, our CNAs were supposed to do the restorative exercises with residents. It's not easy for CNAs to do exercises with a resident if they don't know what they're doing. That opens the door up for me being hurt and I didn't like risking that. So I began refusing restorative on days that I wasn't comfortable doing the exercises with the CNA I had.
In mid-Dec. 2010, while trying to play a trick on my husband, my son taught me how to get myself in and out of bed without assistance from anyone. We were getting ready to go out and my husband stepped outside to clean out my seat in the car. As he was doing that, my CNA came in to help me finish getting ready. She also got me into my wheelchair so that I was ready as soon as my husband came back inside. After she left, my son came up with the idea of telling my husband that he and I got me in my wheelchair, by ourselves. I said he could, but that he'd have to tell Dad the truth eventually. My husband came in and as I knew he would, asked how I got in my chair. I just gave my son a pointed look. He change the subject very fast. A bit later, he said he was ready to show Dad how we got me up. I was waiting to see how much I'd end up hurting because of this. So he told me to lift my legs out in front of my like I did before. I did but didn't raise them up high enough. He said to raise them higher than the bed. Ok.... So I did. And he moved my wheelchair next to the side of the bed so that my legs were laying across the bed from right side to left. He set my brakes and told me to scoot over onto the bed. I gave my husband a look that said "Hey this might work." And he kinda gave me a look that said he agreed. So I scooted forward out of my chair and onto the bed. I had no trouble scooting. I think we were all a bit surprised. So I scooted back into my chair. I had a bit of trouble because the pocket on my jeans caught on the underside of the seat on my wheelchair, but was able to get over that. I just needed to have someone hold the chair so that I did not tip it over. I was so excited. I cannot tell how many people I drug into my room over the next few days to show them what I could do. The ones I didn't drag in, got told. One person I told came in to watch me. Then Donna, who was also my OT, got me a transfer board and anti-tip bars for my wheelchair. She also wanted someone to be with me when I transferred, which I was ok with given she was just watching out for my safety. It got to where I didn't enjoy waiting on people just so I could slide two feet. But I also understood that it was a safety issue.
In early Jan. 2011, an issue happened that caused me to lose my temper and let out everything that had been bothering me. One of the things that came out was the fact that my restorative had become a joke since no one ever worked in restorative it seemed and none of my aides offered to do my restorative. I was doing the exercises on my own some of the time, just to keep up the habit. I was a bit unhappy over the fact that PT did nothing for me other than mess things up. The unit manager changed my restorative to 5 days when she found out I hadn't been getting it the first time. They had also made all of the CNAs watch my restorative so they knew what to do. But, it wasn't being done. And I was at a point that I really thought I needed to move beyond just ROM and stretching. The next day, social services let me know that someone was going to come by and see me to do a PT evaluation. I was thrilled. A bit later, one of the therapists, stopped to see me in the activity room. He asked if he could come by later that afternoon. I said that was fine because "...my son and husband wouldn't be there until around 6:30 or so for my bir....nothing". I caught myself because I didn't want people to know it was my birthday! I am not big on celebrations. So he stopped in, had me show him the things I could do, give him a history of what brought me to the point we were at, my goals etc. He had me transfer from chair to bed and back. He said I did well with that. Then he dropped a bomb on me....a good one though. He ended up giving me a wonderful birthday present. He said he saw no reason for me to need someone with me when I transferred! I was thrilled beyond belief. We also decided that I would go to the therapy dept. the next day to begin my PT. We'd start out low intensity and very slow, that way I did not have any trouble with flaring because of the sudden working of body parts that hadn't worked much at all in recent time. We decided we'd work three days a week and about an hour at a time.
 |
| My left hand prior to OT |
 |
| Left hand with E-Stim electrodes |
 |
| Left and with E-Stim electrodes and hand exerciser |
 | ||
| April 2011Towel Wedge to counter joint contractures |
We then went and had some lunch. Hung out in my room for a little while before it was time for me to go to PT. That was something my son really seemed very excited about. So we went down to the PT dept. and I went ahead and got started on doing my pulley exercises. My son said, "I bet you can't lift 5 pounds on there." Well how could I not take his challenge? I got the weight on the pulley and began to do my exercises. I did them, not easily but I did them. By that time, Jim was ready to begin working with me. So he came over carrying the towels he had made into wedges to compensate for the contractures in my ankles when I first started to stand.These were quite frankly and ingenious idea. Almost everyone on the therapy staff was amazed at Jim's idea. I was thrilled we had a way of getting me moving before I was able to see the orthotist. I think it's better this way, because we KNEW I could walk before getting my braces.
 |
| April 2011 Getting ready to walk |
As Jim got the towels strapped to my feet, he was chatting with my son. Jim asked if he wanted to help us and he was all for it. So Jim told him that he would need to push my wheelchair as close to me as he could without hitting me or bumping me. That way he'd be able to be right in place if I HAD to sit down quickly. But if he bumped me, it could make me stumble. I'd not fall because I was wearing a gait belt and Jim had me. I knew beyond a shadow of a doubt that I'd never fall of Jim could stop it. I ended up walking approximately 14 ft that first time. We were in the parallel bars with Jim walking backwards in front of me, holding onto the gait belt and my son behind me with my wheelchair. I was so thrilled that I made it. But I definitely had to sit down after even that bit of a distance. Those were the first steps I'd walked since Dec. 2008, so they were big steps. We didn't want me to over do it, but I was so excited. Actually, I think everyone in the room was excited for me. Residents, PTs, OTs, the OTAs, PTAs, my son...everyone pretty much beamed, clapped, cheered or just made positive comments. I began walking with a platform walker, then switched to a regular walker.
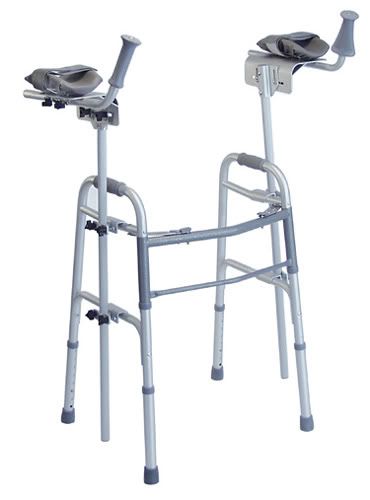 |
| Platform Walker |
As time went by, I became better at walking and we eventually walked in the halls rather than just in the therapy department. As we walked, we'd get stopped by residents so that they could tell me I was doing a great job and then tell Jim how well he did at helping me. Even residents who could not speak for whatever reason, would stop us and grin or give a thumbs up to Jim. It was touching to know I had that many cheerleaders really. That was just residents at the nursing home. That was not the staff. The staff was also extremely excited for me when I began walking again. It brings home the fact that the staff at Conway Manor treats the residents like members of their family. They are so caring about the residents who come in. They make an effort to get to know you. Even to the point of getting to know your family. I know that has to help anyone who comes in and doesn't have the family support that I had. I figure if they treated me like family even with my family being there for me, how much more are the a replacement family for those who have been dropped off and left like you would take an unwanted animal to the pound? I know even the hardest of people to get along with had people that they would respond to. And those people worked hard to get a response, but when they did, it was usually the start of a special relationship.
 |
| May 2011 Bilateral ankle-foot orthoses before removing plastic calf support and adding T-straps at ankles |
I progressed throughout the summer, especially after I got my bilateral ankle-foot orthoses (AFOs) with T-straps, and heel lifts to compensate for my ankle contractures. Dr. Alexander Lyons, of Lyons Prosthetics and Orthotics and his staff were awesome! Dr Lyons was the first doctor who, during an outpatient office visit, offered to pray with me before we began the appointment. I was amazed. I'd had surgeons pray before surgery. One of the doctors at the hospital prayed with and for me often. I know one day, I woke up to him praying for me. Having a doctor pray prior to doing anything invasive doesn't seem too out of the ordinary to me. But, a doctor praying at the start of an office visit is a pleasant surprise. I've been blessed not only with great doctors but also doctors who seem to have faith and not be afraid to show it. The right shoe's insole insert was slightly padded on the underside to prevent the tips of the toes on my foot from rubbing on the inner sole of the show. The padding was added in Sept. after I had a problem with the big toe on my right foot. Due to joint contractures, all of the toes on my right foot have something wrong with them. A couple are bent in a way that when I put my foot on the floor (as best as I can), I basically stand with all of my weight on the tips of my toes. I didn't feel the sore forming because of the decreased sensation in my feet because of the peripheral neuropathy. I generally did look at my feet from time to time, but because I can't bend well enough to see the tips of my toes on my right foot, I never thought to have someone else take a look to make sure there were no problems. By the time I felt the pain from the sore, it was a bit deep and had what everyone who saw it described as a "hole" in my toe. Yay! I was off my feet for much of Sept. Once Dr Lyons fixed the insole of my shoe so that the toe no longer rubbed, it only took a couple of weeks for me to be able to tolerate wearing the AFOs. But, even as late as Jan. 2012, it was still not fully healed. There was a piece of dry skin that came off of the tip of my toe that had a hole about 1/8" in diameter in it. I cannot imagine how big it was BEFORE it had healed up. I don't even want to know how deep it was. I almost think that the tip of that toe is a bit more sensitive now, it's either that or I am just paying more attention to how the toes feel. I now have my hubby at least peek at the tips of my toes once in awhile. Or when I shower I sit on my shower chair with my legs outside the tub and straight out in front of me so I can see them in the mirror on the back of the bathroom door. Even so, that's not the best way because I can't see it close up.
 |
| Sept. 2011 Right big toe the reddest area on the tip is where the hole ended up. |
 |
| Loftstrand AKA forearm or Canadian crutches |
I am so very thankful to be home. I owe a lot of gratitude to all of the various people cared for me during the time I was sick and re-learning all the everyday things most people take for granted. I mean, come on, how many people does it take to blow my nose? There for awhile...it took at least 3, one to hold me in an upright position, one to hold the tissue to my nose and then me to actually blow. Same with a number of activities that people do on a daily basis for themselves. I was unable to do many things for myself and so have a bunch of people who helped me through that rough period. I also have a number of people to thank for just believing in me enough to make sure I got my PT and got the help I needed to get me on my feet and able to take those first steps in over two years. Having the wonderful support that I did, how could I do anything but succeed? I went from being in the hospital and not being alert or oriented, unable to remember things, unable to sit up for more than 2 minutes, unable to do anything for myself, etc....
 | |
| At Grand Strand Regional Medical Center Spring 2009 |
 |
| At home Spring 2012 |
I am so very grateful for everyone who had a hand in my care. I was blessed to have relatively few problems with staff members who were not quite tolerable. I might have been a nightmare patient to some people because I expected people to do their jobs and to do them properly. I did not take well to people treating me as if there was something wrong with me mentally and was why I was in the nursing home. Neither did I let staff members slack off when it came to their care of my roommates, especially those who could not speak up for themselves. I did not hesitate to go to the unit manager or Social Services if there was a problem I couldn't fix on my own. I honestly tried to keep problems between myself and the person I was having the problem with, but when repeated attempts and requests did not get my point across, then it was time to seek more help. I had two CNAs that I had serious issues with. With each of them, the issue was the pain they caused me. In the hospital, I was a lot more sensitive to pain because I was not on my RA meds and even with morphine, my pain levels were horrendously high. At the nursing home, I was back on my RA meds as well as back on methadone for pain. I have found it to be the best pain medication for me and so I was not as sensitive to pain. In the hospital, even the gentlest of touches brought on tears. At the nursing home, it took more than that to make me hurt just by touching me. But there was one aide that I argued with for MONTHS over me asking her, then telling her to please be more gentle, that she was rough with me, that she was hurting me, etc. etc. And she had the nerve to tell me that there was NO WAY she could be hurting me. I apparently was too stupid to know what was painful simply because I was in a nursing home, I guess. In the hospital, my Mom took care of the issue by speaking to the charge nurse that she did not want that aide caring for me any longer. They honored that request, until fall when all the aides went back to school. But they at least asked me if I would let her care for me and then decide from there. I was fine with that, and she did fine. She didn't hurt me, except when something was painful no matter who did it or how they did it, such as washing my feet. That was completely unavoidable and in fact, still hurts quite a bit. At the nursing home, the aide that was the problem kept telling me there was no way she was hurting me, that no one else complained about her being rough with them (I never said this but I wondered to myself if they didn't speak up because they were afraid of her?) and that she...blah blah blah...I tuned her out. Other than those incidents, the staff at both the hospital and the nursing home were wonderful. I am so grateful for the friends I made at both places. I keep in touch with some of them on Facebook. I also see the nursing home staff when I go back out a couple Fridays a month for Bible study and visitation. It's as if I am a long lost family member coming home when I go to the nursing home. The residents also make me feel missed and loved. Even a few staff members who are no longer at the Manor are friends of mine. I am so thankful that I had Jim to work with. Had he not been the inventive person he is, my therapy would have been delayed until July basically. We got the jump on me walking because he thought of the towels, otherwise I would have had to wait on my braces. Jim is the supportive type. He knew when to push me and when I needed held back. He often stopped me from doing more than I needed to be doing and causing myself a flare. He could take a look at me and know if I just did not feel well, or when it was time for me to either stop what we were doing or at least slow down or switch activities.Jim was so very modest. Anytime I tried to express my thank for all that he had done, he kinda brushed it off as just doing his job or made a bit of a joke about it. One day, as we were walking, we stopped to speak to a relatively new employee. Talk turned to me walking and she commented on how well I was doing. I spoke up and commented on how we started with the towels, which is is something I tend to tell people about because I think it was such an awesome idea. His reply on the subject? "Oh I stayed at a Holiday Inn last night!"
I am so glad things turned out the way they did. I am convinced things happen for a reason and now it's just about a matter of using the lessons I learned throughout this time.

No comments:
Post a Comment